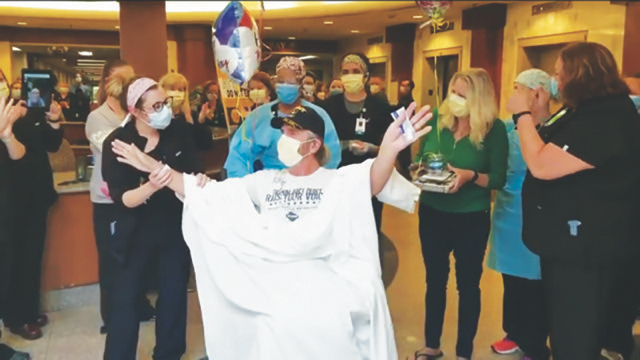
‘Code Sunshine’ is a welcome birthday gift: After being admitted for COVID-19 to Mercy Hospital South on his daughter’s birthday, April 2, Bill finally went home last week with his wife, Lynn – on his own 68th birthday. Bill, a COVID-19 patient who only wanted to provide his first name, spent three weeks at Mercy Hospital South, with a week on a ventilator and two weeks in intensive care. He was treated with convalescent plasma donated by someone recovered from COVID-19. Mercy South calls a ‘Code Sunshine’ to celebrate with COVID-19 patients as they leave the hospital. After Bill left through the lobby with Lynn to cheers from workers lining the halls, some of his nurses and therapists signed his shirt with their motto ‘Stayin’ Alive.’
Mercy Hospital South is overwhelmed with COVID-19 patients even before an expected post-Thanksgiving surge, taking a toll on staff and, if many more ambulances roll up, perhaps leading to decisions on who will be able to receive care or not.
The hospital formerly known as St. Anthony’s is anticipating a wave of hospitalizations this week following holiday gatherings, part of an unprecedented four-week wave of cases that is unlike anything the hospital has ever seen and more akin to wartime than what Americans are used to seeing in a hospital, said Mercy South Chief Medical Officer Dr. Aamina Akhtar.
The current wave of cases is double the number that Mercy South saw in March when the pandemic first hit, said Akhtar, who said Mercy South has the highest number of COVID-19 patients of any Mercy and possibly St. Louis hospital on a per-bed basis, and the hospital is the only Mercy hospital that has considered ending all elective procedures in order to clear more space and doctors, but as of now the hospital is trying to balance scheduled surgeries with the influx of COVID-19 patients it is seeing every day. The hospital has turned some postoperative rooms into intensive-care units and is considering turning some postpartum rooms into more floor units. COVID-19 patients who are not as sick and only need oxygen are sent home and monitored under a new program.
The most difficult challenge beyond just finding space for an unprecedented number of sick patients is finding nurses and doctors to properly care for them, even as those patients are sicker and require more care than the hospital’s typical patient.
“We will have four weeks of a crisis in health care beyond anything that we’ve ever seen in our lifetimes, but I’m hoping that as that becomes more visible and people who are concerned about the reality of what was happening, as we get people who are not able to get to the hospital for heart attacks or broken bones just because we are beyond any means of capacity or labor to help people — that gives us an opportunity to change not these four weeks but beyond that and at least minimize the severity or the length that we see this crisis,” said Akhtar.
Although the situation can appear hopeless, Akhtar encourages anyone who is not yet wearing a mask to start now so that future hospitalizations can be prevented. Hospitalizations trail a few weeks after a wave of cases, so wearing a mask now will prevent hospitalizations in January.
“It’s not a tidal wave coming at us, it’s kind of a tsunami,” Akhtar said, noting that hospital leaders have been warning all year that the time might come: “We’ve been saying this for awhile and hoping that local leaders and community members would take heed and mask — that’s what makes the biggest difference. And it wasn’t taken seriously to the extent that we wanted nor were policies in place that would have prevented this, so we don’t have a choice. The best thing we can do for the next four weeks is emergency disaster planning.”
When South County state legislators announced they will sponsor bills to take away St. Louis County’s power to enact stay-at-home orders, Sen. Andrew Koenig noted that a state website lists only half the hospital beds filled. Koenig — whose district includes Mercy South — said that hospitals have plenty of capacity, unlike what their leaders are saying.
“This is also false information,” Koenig said Dec. 1, referring to hospital capacity.
But Dr. Alex Garza, the head of the St. Louis Metropolitan Pandemic Task Force, gave an analogy to illustrate how the discrepancy arises.
“When we look at capacity, we look at the number of beds we can staff, not the number of beds we have,” Garza said Nov. 6. “If I only have staff for 800 beds, then our capacity is for 800 patients. If I have 100 buses, if I’ve only got one driver I’ve only got one bus.”
Even in an apples-to-apples comparison of COVID-19 versus the same number of non-COVID patients, hospital staffers are more stressed and overworked when caring for a COVID-19 patient.
The shortage of doctors and nurses is really what is hitting hospitals the hardest now, said Akhtar. She said if someone could send her resumes of available nurses and doctors, she would be “happy to hire them on the spot.” Any nurses and doctors who were furloughed or part of layoffs earlier this year are now back to work. The nursing shortage predated COVID-19, but the hospital is “feeling it more acutely now,” Akhtar noted. Hospitals are looking for nurses through agencies and even internationally. During the March wave in New York, for example, nurses came from all over the country to help hospitals overwhelmed by that surge. But now with cases rising in every single state and everywhere a hotspot for the coronavirus, there are no extra nurses to come to St. Louis to help.
“To be honest you could give us 1,000 more beds for patients, but what we don’t have is a labor force to take care of them — whether it be physicians or nursing or respiratory therapists — and that’s what’s going to really not just stretch but overwhelm our ability to take care of people,” Akhtar said.
To cope with its inundated staff, Mercy South is turning to a “pyramid model of care” — instead of one ICU doctor taking care of 10 patients as would usually happen, now two pulmonary doctors might oversee 10 patients each and report about the 20 patients to the ICU doctor. That is approaching “crisis standard of care,” where the hospital decides who gets care.
“When you have limited resources, and you have patients that exceed that, as health care workers it’s our worst nightmare,” said Akhtar. “We will have to make decisions about who gets health care, and it’s unfortunate that in the United States in 2020 we will not be able to take care of patients like we want to and will have to pick and choose who gets a vent, who gets Remdesivir, who gets steroids — that’s what we’re facing right now.”